What Can You Do About Fallen Arches?
Overview
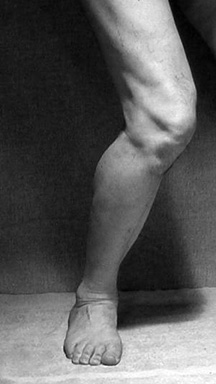
A normal foot should arch so the middle of the foot does not touch the ground when the patient stands up. If it does touch, the patient has a flat foot or fallen arch. Flat feet are normal for young children. Their arches should develop by adulthood, but sometimes they fail to develop. Some people with flat feet have pain in the heel or arch, but others do not.
Causes
There are several reasons why arches fall. It can be genetic, it can be a result of unsupported shoes, a product of our lives and the pressure we put on the feet. Some people have active lifestyles so the wear and tear effect on the muscles there that runs down the back of the calf and wraps around the arch can slacken as we get older. It can be a number of things.
Symptoms
The primary symptom of flatfeet is the absence of an arch upon standing. Additional signs of flatfeet include the following. Foot pain. Pain or weakness in the lower legs. Pain or swelling on the inside of the ankle. Uneven shoe wear. While most cases of flatfeet do not cause problems, complications can sometimes occur. Complications include the following, bunions and calluses, inability to walk or run normally, inflammation and pain in the bottom of the foot (plantar fasciitis), tendonitis in the Achilles heel and other ligaments, pain in the ankles, knees, and hips due to improper alignment, shin splints, stress fractures in the lower legs.
Diagnosis
Runners are often advised to get a gait analysis to determine what type of foot they have and so what kind of running shoe they require. This shouldn?t stop at runners. Anyone that plays sports could benefit from this assessment. Sports shoes such as football boots, astro trainers and squash trainers often have very poor arch support and so for the 60-80% of us who do overpronate or have flat feet they are left unsupported. A change of footwear or the insertion of arch support insoles or orthotics can make a massive difference to your risk of injury, to general aches and pains and even to your performance.
no-foot-pain.com
Non Surgical Treatment
Most cases of fallen arches are not painful and need no form of treatment. However, common symptoms of fallen arches can include pain in your feet (particularly in the area of your heel or arch), pain in your feet that persists after long bouts of physical activity or standing up, achy feet, or arch pain when standing on the tips of your toes. Most cases of fallen arches are not preventable. Treatments for fallen arches include, rest, ice, compression, medication to relieve pain, orthotics, or in some cases surgery.
Surgical Treatment

Common indications for surgery are cerebral palsy with an equinovalgus foot, to prevent progression and breakdown of the midfoot. Rigid and painful Pes Planus. To prevent progression, eg with a Charcot joint. Tibialis posterior dysfunction, where non-surgical treatment is unsuccessful. Possible surgical procedures include Achilles tendon lengthening. Calcaneal osteotomy, to re-align the hindfoot. Reconstruction of the tibialis posterior tendon. For severe midfoot collapse of the arch, triple arthrodesis may be indicated.
Prevention
oll away pain. If you're feeling pain in the arch area, you can get some relief by massaging the bottom of your foot. A regular massage while you're watching TV can do wonders" Stretch out. Doing the same type of stretching exercises that runners do in their warm-up can help reduce arch pain caused by a tight heel cord. One of the best exercises is to stand about three feet from a wall and place your hands on the wall. Leaning toward the wall, bring one foot forward and bend the knee so that the calf muscles of the other leg stretch. Then switch legs. Stretching is particularly important for women who spend all week in heels and then wear exercise shoes or sneakers on weekends. Get measured each time you buy new shoes. Don't assume that since you always wore a particular size, you always will. Too many people try to squeeze into their 'regular' shoe size and wind up with serious foot problems or sores on their feet. When your arch is falling, your feet may get longer or wider and you may or may not feel pain, so getting your foot measured each time you buy shoes is a good indicator of your arch's degeneration. Examine your shoes. If the heel is worn down, replace it. But if the back portion of the shoe is distorted or bent to one side, get yourself into a new pair of supportive shoes like those made specifically for walking. That's because flat feet can affect your walking stride, and failing to replace worn shoes may lead to knee or hip pain.
After Care
Time off work depends on the type of work as well as the surgical procedures performed. . A patient will be required to be non-weight bearing in a cast or splint and use crutches for four to twelve weeks. Usually a patient can return to work in one to two weeks if they are able to work while seated. If a person's job requires standing and walking, return to work may take several weeks. Complete recovery may take six months to a full year. Complications can occur as with all surgeries, but are minimized by strictly following your surgeon's post-operative instructions. The main complications include infection, bone that is slow to heal or does not heal, progression or reoccurrence of deformity, a stiff foot, and the need for further surgery. Many of the above complications can be avoided by only putting weight on the operative foot when allowed by your surgeon.

A normal foot should arch so the middle of the foot does not touch the ground when the patient stands up. If it does touch, the patient has a flat foot or fallen arch. Flat feet are normal for young children. Their arches should develop by adulthood, but sometimes they fail to develop. Some people with flat feet have pain in the heel or arch, but others do not.
Causes
There are several reasons why arches fall. It can be genetic, it can be a result of unsupported shoes, a product of our lives and the pressure we put on the feet. Some people have active lifestyles so the wear and tear effect on the muscles there that runs down the back of the calf and wraps around the arch can slacken as we get older. It can be a number of things.
Symptoms
The primary symptom of flatfeet is the absence of an arch upon standing. Additional signs of flatfeet include the following. Foot pain. Pain or weakness in the lower legs. Pain or swelling on the inside of the ankle. Uneven shoe wear. While most cases of flatfeet do not cause problems, complications can sometimes occur. Complications include the following, bunions and calluses, inability to walk or run normally, inflammation and pain in the bottom of the foot (plantar fasciitis), tendonitis in the Achilles heel and other ligaments, pain in the ankles, knees, and hips due to improper alignment, shin splints, stress fractures in the lower legs.
Diagnosis
Runners are often advised to get a gait analysis to determine what type of foot they have and so what kind of running shoe they require. This shouldn?t stop at runners. Anyone that plays sports could benefit from this assessment. Sports shoes such as football boots, astro trainers and squash trainers often have very poor arch support and so for the 60-80% of us who do overpronate or have flat feet they are left unsupported. A change of footwear or the insertion of arch support insoles or orthotics can make a massive difference to your risk of injury, to general aches and pains and even to your performance.
no-foot-pain.com
Non Surgical Treatment
Most cases of fallen arches are not painful and need no form of treatment. However, common symptoms of fallen arches can include pain in your feet (particularly in the area of your heel or arch), pain in your feet that persists after long bouts of physical activity or standing up, achy feet, or arch pain when standing on the tips of your toes. Most cases of fallen arches are not preventable. Treatments for fallen arches include, rest, ice, compression, medication to relieve pain, orthotics, or in some cases surgery.
Surgical Treatment

Common indications for surgery are cerebral palsy with an equinovalgus foot, to prevent progression and breakdown of the midfoot. Rigid and painful Pes Planus. To prevent progression, eg with a Charcot joint. Tibialis posterior dysfunction, where non-surgical treatment is unsuccessful. Possible surgical procedures include Achilles tendon lengthening. Calcaneal osteotomy, to re-align the hindfoot. Reconstruction of the tibialis posterior tendon. For severe midfoot collapse of the arch, triple arthrodesis may be indicated.
Prevention
oll away pain. If you're feeling pain in the arch area, you can get some relief by massaging the bottom of your foot. A regular massage while you're watching TV can do wonders" Stretch out. Doing the same type of stretching exercises that runners do in their warm-up can help reduce arch pain caused by a tight heel cord. One of the best exercises is to stand about three feet from a wall and place your hands on the wall. Leaning toward the wall, bring one foot forward and bend the knee so that the calf muscles of the other leg stretch. Then switch legs. Stretching is particularly important for women who spend all week in heels and then wear exercise shoes or sneakers on weekends. Get measured each time you buy new shoes. Don't assume that since you always wore a particular size, you always will. Too many people try to squeeze into their 'regular' shoe size and wind up with serious foot problems or sores on their feet. When your arch is falling, your feet may get longer or wider and you may or may not feel pain, so getting your foot measured each time you buy shoes is a good indicator of your arch's degeneration. Examine your shoes. If the heel is worn down, replace it. But if the back portion of the shoe is distorted or bent to one side, get yourself into a new pair of supportive shoes like those made specifically for walking. That's because flat feet can affect your walking stride, and failing to replace worn shoes may lead to knee or hip pain.
After Care
Time off work depends on the type of work as well as the surgical procedures performed. . A patient will be required to be non-weight bearing in a cast or splint and use crutches for four to twelve weeks. Usually a patient can return to work in one to two weeks if they are able to work while seated. If a person's job requires standing and walking, return to work may take several weeks. Complete recovery may take six months to a full year. Complications can occur as with all surgeries, but are minimized by strictly following your surgeon's post-operative instructions. The main complications include infection, bone that is slow to heal or does not heal, progression or reoccurrence of deformity, a stiff foot, and the need for further surgery. Many of the above complications can be avoided by only putting weight on the operative foot when allowed by your surgeon.
Heel Soreness
Overview

Plantar fasciitis is the most common cause of heel pain. The plantar fascia, a band of tough tissue connecting the heel bone to the toes, becomes irritated or inflamed. Heel pain, worst in the morning when getting out of bed, is the most common symptom. Arch pain may also be present. Heel spurs are abnormal growths of bone on the bottom of the heel bone that may be caused by an abnormal gait, posture or walking, inappropriate shoes, or certain activities, like running. Spurs may cause foot pain while walking or standing. Although one in 10 people has heel spurs, only one in 20 of these people will have foot pain. Heel spurs can occur in people with plantar fasciitis, but they do not cause plantar fasciitis. People with flat feet or high arches are more likely to have foot pain from heel spurs.
Causes
Heel pain is not usually caused by a single injury, such as a twist or fall, but rather the result of repetitive stress and pounding of the heel. The most common causes of heel pain are Plantar fasciitis (plantar fasciosis) - inflammation of the plantar fascia. The plantar fascia is a strong bowstring-like ligament that runs from the calcaneum (heel bone) to the tip of the foot. When the plantar fasciitis is stretched too far its soft tissue fibers become inflamed, usually where it attaches to the heel bone. Sometimes the problem may occur in the middle of the foot. The patient experiences pain under the foot, especially after long periods of rest. Some patients have calf-muscle cramps if the Achilles tendon tightens too. Heel bursitis, inflammation of the back of the heel, the bursa (a fibrous sac full of fluid). Can be caused by landing awkwardly or hard on the heels. Can also be caused by pressure from footwear. Pain is typically felt either deep inside the heel or at the back of the heel. Sometimes the Achilles tendon may swell. As the day progresses the pain usually gets worse. Heel bumps (pump bumps) common in teenagers. The heel bone is not yet fully mature and rubs excessively, resulting in the formation of too much bone. Often caused by having a flat foot. Among females can be caused by starting to wear high heels before the bone is fully mature Tarsal tunnel syndrome, a large nerve in the back of the foot becomes pinched, or entrapped (compressed). This is a type of compression neuropathy that can occur either in the ankle or foot. Chronic inflammation of the heel pad, caused either by the heel pad becoming too thin, or heavy footsteps. Stress fracture, this is a fracture caused by repetitive stress, commonly caused by strenuous exercise, sports or heavy manual work. Runners are particularly prone to stress fracture in the metatarsal bones of the foot. Can also be caused by osteoporosis. Severs disease (calcaneal apophysitis) the most common cause of heel pain in child/teenage athletes, caused by overuse and repetitive microtrauma of the growth plates of the calcaneus (heel bone). Children aged from 7-15 are most commonly affected. Achilles tendonosis (degenerative tendinopathy) also referred to as tendonitis, tendinosis and tendinopathy. A chronic (long-term) condition associated with the progressive degeneration of the Achilles tendon. Sometimes the Achilles tendon does not function properly because of multiple, minor microscopic tears of the tendon, which cannot heal and repair itself correctly, the Achilles tendon receives more tension than it can cope with and microscopic tears develop. Eventually, the tendon thickens, weakens and becomes painful.
Symptoms
Symptoms may also include swelling that is quite tender to the touch. Standing, walking and constrictive shoe wear typically aggravate symptoms. Many patients with this problem are middle-aged and may be slightly overweight. Another group of patients who suffer from this condition are young, active runners.
Diagnosis
The diagnosis of heel pain and heel spurs is made by a through history of the course of the condition and by physical exam. Weight bearing x-rays are useful in determining if a heel spur is present and to rule out rare causes of heel pain such as a stress fracture of the heel bone, the presence of bone tumors or evidence of soft tissue damage caused by certain connective tissue disorders.
Non Surgical Treatment
Initially, treatment will consist of adding support to the foot, including better shoes and an over-the-counter arch supports and/or insoles; resting from the sport or activity that aggravates the problem; stretching the calf and arch muscles; taking anti-inflammatory; and using ice and massage to reduce inflammation. You can ice and message your muscles simultaneously by freezing a water bottle filled with water and using it to massage your foot by rolling it underneath your foot for five to 10 minutes at least two times per day. It is not unusual for symptoms of plantar fasciitis to persist for six to 12 months despite treatment.
Surgical Treatment
Extracorporeal shockwave therapy (EST) is a fairly new type of non-invasive treatment. Non-invasive means it does not involve making cuts into your body. EST involves using a device to deliver high-energy soundwaves into your heel. The soundwaves can sometimes cause pain, so a local anaesthetic may be used to numb your heel. It is claimed that EST works in two ways. It is thought to have a "numbing" effect on the nerves that transmit pain signals to your brain, help stimulate and speed up the healing process. However, these claims have not yet been definitively proven. The National Institute for Health and Care Excellence (NICE) has issued guidance about the use of EST for treating plantar fasciitis. NICE states there are no concerns over the safety of EST, but there are uncertainties about how effective the procedure is for treating heel pain. Some studies have reported that EST is more effective than surgery and other non-surgical treatments, while other studies found the procedure to be no better than a placebo (sham treatment).
heel pain exercises
Prevention

A variety of steps can be taken to avoid heel pain and accompanying afflictions. Wear shoes that fit well-front, back, and sides-and have shock-absorbent soles, rigid shanks, and supportive heel counters. Wear the proper shoes for each activity. Do not wear shoes with excessive wear on heels or soles. Prepare properly before exercising. Warm up and do stretching exercises before and after running. Pace yourself when you participate in athletic activities. Don't underestimate your body's need for rest and good nutrition. If obese, lose weight.

Plantar fasciitis is the most common cause of heel pain. The plantar fascia, a band of tough tissue connecting the heel bone to the toes, becomes irritated or inflamed. Heel pain, worst in the morning when getting out of bed, is the most common symptom. Arch pain may also be present. Heel spurs are abnormal growths of bone on the bottom of the heel bone that may be caused by an abnormal gait, posture or walking, inappropriate shoes, or certain activities, like running. Spurs may cause foot pain while walking or standing. Although one in 10 people has heel spurs, only one in 20 of these people will have foot pain. Heel spurs can occur in people with plantar fasciitis, but they do not cause plantar fasciitis. People with flat feet or high arches are more likely to have foot pain from heel spurs.
Causes
Heel pain is not usually caused by a single injury, such as a twist or fall, but rather the result of repetitive stress and pounding of the heel. The most common causes of heel pain are Plantar fasciitis (plantar fasciosis) - inflammation of the plantar fascia. The plantar fascia is a strong bowstring-like ligament that runs from the calcaneum (heel bone) to the tip of the foot. When the plantar fasciitis is stretched too far its soft tissue fibers become inflamed, usually where it attaches to the heel bone. Sometimes the problem may occur in the middle of the foot. The patient experiences pain under the foot, especially after long periods of rest. Some patients have calf-muscle cramps if the Achilles tendon tightens too. Heel bursitis, inflammation of the back of the heel, the bursa (a fibrous sac full of fluid). Can be caused by landing awkwardly or hard on the heels. Can also be caused by pressure from footwear. Pain is typically felt either deep inside the heel or at the back of the heel. Sometimes the Achilles tendon may swell. As the day progresses the pain usually gets worse. Heel bumps (pump bumps) common in teenagers. The heel bone is not yet fully mature and rubs excessively, resulting in the formation of too much bone. Often caused by having a flat foot. Among females can be caused by starting to wear high heels before the bone is fully mature Tarsal tunnel syndrome, a large nerve in the back of the foot becomes pinched, or entrapped (compressed). This is a type of compression neuropathy that can occur either in the ankle or foot. Chronic inflammation of the heel pad, caused either by the heel pad becoming too thin, or heavy footsteps. Stress fracture, this is a fracture caused by repetitive stress, commonly caused by strenuous exercise, sports or heavy manual work. Runners are particularly prone to stress fracture in the metatarsal bones of the foot. Can also be caused by osteoporosis. Severs disease (calcaneal apophysitis) the most common cause of heel pain in child/teenage athletes, caused by overuse and repetitive microtrauma of the growth plates of the calcaneus (heel bone). Children aged from 7-15 are most commonly affected. Achilles tendonosis (degenerative tendinopathy) also referred to as tendonitis, tendinosis and tendinopathy. A chronic (long-term) condition associated with the progressive degeneration of the Achilles tendon. Sometimes the Achilles tendon does not function properly because of multiple, minor microscopic tears of the tendon, which cannot heal and repair itself correctly, the Achilles tendon receives more tension than it can cope with and microscopic tears develop. Eventually, the tendon thickens, weakens and becomes painful.
Symptoms
Symptoms may also include swelling that is quite tender to the touch. Standing, walking and constrictive shoe wear typically aggravate symptoms. Many patients with this problem are middle-aged and may be slightly overweight. Another group of patients who suffer from this condition are young, active runners.
Diagnosis
The diagnosis of heel pain and heel spurs is made by a through history of the course of the condition and by physical exam. Weight bearing x-rays are useful in determining if a heel spur is present and to rule out rare causes of heel pain such as a stress fracture of the heel bone, the presence of bone tumors or evidence of soft tissue damage caused by certain connective tissue disorders.
Non Surgical Treatment
Initially, treatment will consist of adding support to the foot, including better shoes and an over-the-counter arch supports and/or insoles; resting from the sport or activity that aggravates the problem; stretching the calf and arch muscles; taking anti-inflammatory; and using ice and massage to reduce inflammation. You can ice and message your muscles simultaneously by freezing a water bottle filled with water and using it to massage your foot by rolling it underneath your foot for five to 10 minutes at least two times per day. It is not unusual for symptoms of plantar fasciitis to persist for six to 12 months despite treatment.
Surgical Treatment
Extracorporeal shockwave therapy (EST) is a fairly new type of non-invasive treatment. Non-invasive means it does not involve making cuts into your body. EST involves using a device to deliver high-energy soundwaves into your heel. The soundwaves can sometimes cause pain, so a local anaesthetic may be used to numb your heel. It is claimed that EST works in two ways. It is thought to have a "numbing" effect on the nerves that transmit pain signals to your brain, help stimulate and speed up the healing process. However, these claims have not yet been definitively proven. The National Institute for Health and Care Excellence (NICE) has issued guidance about the use of EST for treating plantar fasciitis. NICE states there are no concerns over the safety of EST, but there are uncertainties about how effective the procedure is for treating heel pain. Some studies have reported that EST is more effective than surgery and other non-surgical treatments, while other studies found the procedure to be no better than a placebo (sham treatment).
heel pain exercises
Prevention

A variety of steps can be taken to avoid heel pain and accompanying afflictions. Wear shoes that fit well-front, back, and sides-and have shock-absorbent soles, rigid shanks, and supportive heel counters. Wear the proper shoes for each activity. Do not wear shoes with excessive wear on heels or soles. Prepare properly before exercising. Warm up and do stretching exercises before and after running. Pace yourself when you participate in athletic activities. Don't underestimate your body's need for rest and good nutrition. If obese, lose weight.
Heel Lifts For Leg Length Discrepancy
Overview
Limb-length discrepancies or differences are conditions that result in limbs that are unequal in length or that exhibit other anomalies. The conditions occur when bones or joints in the arms or legs are abnormal or become damaged. Providers might refer to these conditions as limb-length discrepancies, limb differences or limb-length conditions.
Causes
Leg discrepancy can develop from a medical issue in any portion of the femur or tibia. One leg may lengthen, but leg shortening is much more common. Factors that can cause leg length discrepancy include inherited growth deficiencies. Infections. A bone infection can cause delayed growth in the affected limb. Injury. If your child breaks a leg, it may be shorter once it heals. This is most likely to happen if the fracture or break was complicated, an open fracture, or an injury that affected the growth plate near the end of the bone. Alternatively, a break can cause bones to grow faster after healing, making a leg longer. Tumors. Legg-Calve-Perthes disease. This is a condition that affects the ball (femoral head) of the hip joint. The femoral head may be friable and damage easily, sometimes leading to shortening of the thigh bone. Hemihypertrophy. In children with this condition, one side of the body grows more quickly than the other. Vascular malformations. These are abnormal clusters of veins and arteries that can form close to the bone and stimulate growth. Juvenile arthritis. Inflammation from arthritis can stimulate growth in the affected leg and cause discrepancy.
Symptoms
Often there are few or no symptoms prior to the age of 25-35. The most common symptom is chronic lower back pain, but also is frequently middle and upper back pain. Same-sided and repeated injury or pain to the hip, knee and/or ankle is also a hallmark of a long-standing untreated LLD. It is not uncommon to have buttock or radiating hip pain that is non-dermatomal (not from a disc) and tends to go away when lying down.
Diagnosis
On standing examination one iliac crest may be higher/lower than the other. However a physiotherapist, osteopath or chiropractor will examine the LLD in prone or supine position and measure it, confirming the diagnosis of structural (or functional) LLD. The LLD should be measured using bony fixed points. X-Ray should be taken in a standing position. The osteopath, physiotherapist or chiropractor will look at femoral head & acetabulum, knee joints, ankle joints.
Non Surgical Treatment
The non-surgical intervention is mainly usedfor the functional and environmental types of leg length discrepancies. It is also applied to the mild category of limb length inequality. Non-surgical intervention consists of stretching the muscles of the lower extremity. This is individually different, whereby the M. Tensor Fascia latae, the adductors, the hamstring muscles, M. piriformis and M. Iliopsoas are stretched. In this non-surgical intervention belongs also the use of shoe lifts. These shoe lifts consists of either a shoe insert (up to 10-20mm of correction), or building up the sole of the shoe on the shorter leg (up to 30-60mm of correction). This lift therapy should be implemented gradually in small increments. Several studies have examined the treatment of low back pain patients with LLD with shoe lifts. Gofton obtained good results: the patients experienced major or complete pain relief that lasted upon follow-up ranging from 3 to 11 years. Helliwell also observed patients whereby 44% experienced complete pain relief, and 45% had moderate or substantial pain relief. Friberg found that 157 (of 211) patients with LBP, treated with shoe lifts, were symprom-free after a mean follow-up of 18 months.

leg length discrepancy measurement
Surgical Treatment
Leg shortening is employed when LLD is severe and when a patient has already reached skeletal maturity. The actual surgery is called an osteotomy , which entails the removal of a small section of bone in the tibia (shinbone) and sometimes the fibula as well, resulting in the loss of around an inch in total height. Leg lengthening is a difficult third option that has traditionally had a high complication rate. Recently, results have improved somewhat with the emergence of a technique known as callotasis , in which only the outer portion of the bone (the cortex ) is cut, (i.e. a corticotomy ). This allows the bone to be more easily lengthened by an external fixation device that is attached to either side of the cut bone with pins through the skin. The ?ex-fix,' as it is sometimes called, is gradually adjusted by an orthopaedic surgeon, and healing can occur at the same time that the leg is being distracted , or lengthened over time. Unlike epiphysiodesis, leg lengthening procedures can be performed at almost any skeletal or chronological age.
Limb-length discrepancies or differences are conditions that result in limbs that are unequal in length or that exhibit other anomalies. The conditions occur when bones or joints in the arms or legs are abnormal or become damaged. Providers might refer to these conditions as limb-length discrepancies, limb differences or limb-length conditions.

Causes
Leg discrepancy can develop from a medical issue in any portion of the femur or tibia. One leg may lengthen, but leg shortening is much more common. Factors that can cause leg length discrepancy include inherited growth deficiencies. Infections. A bone infection can cause delayed growth in the affected limb. Injury. If your child breaks a leg, it may be shorter once it heals. This is most likely to happen if the fracture or break was complicated, an open fracture, or an injury that affected the growth plate near the end of the bone. Alternatively, a break can cause bones to grow faster after healing, making a leg longer. Tumors. Legg-Calve-Perthes disease. This is a condition that affects the ball (femoral head) of the hip joint. The femoral head may be friable and damage easily, sometimes leading to shortening of the thigh bone. Hemihypertrophy. In children with this condition, one side of the body grows more quickly than the other. Vascular malformations. These are abnormal clusters of veins and arteries that can form close to the bone and stimulate growth. Juvenile arthritis. Inflammation from arthritis can stimulate growth in the affected leg and cause discrepancy.
Symptoms
Often there are few or no symptoms prior to the age of 25-35. The most common symptom is chronic lower back pain, but also is frequently middle and upper back pain. Same-sided and repeated injury or pain to the hip, knee and/or ankle is also a hallmark of a long-standing untreated LLD. It is not uncommon to have buttock or radiating hip pain that is non-dermatomal (not from a disc) and tends to go away when lying down.
Diagnosis
On standing examination one iliac crest may be higher/lower than the other. However a physiotherapist, osteopath or chiropractor will examine the LLD in prone or supine position and measure it, confirming the diagnosis of structural (or functional) LLD. The LLD should be measured using bony fixed points. X-Ray should be taken in a standing position. The osteopath, physiotherapist or chiropractor will look at femoral head & acetabulum, knee joints, ankle joints.
Non Surgical Treatment
The non-surgical intervention is mainly usedfor the functional and environmental types of leg length discrepancies. It is also applied to the mild category of limb length inequality. Non-surgical intervention consists of stretching the muscles of the lower extremity. This is individually different, whereby the M. Tensor Fascia latae, the adductors, the hamstring muscles, M. piriformis and M. Iliopsoas are stretched. In this non-surgical intervention belongs also the use of shoe lifts. These shoe lifts consists of either a shoe insert (up to 10-20mm of correction), or building up the sole of the shoe on the shorter leg (up to 30-60mm of correction). This lift therapy should be implemented gradually in small increments. Several studies have examined the treatment of low back pain patients with LLD with shoe lifts. Gofton obtained good results: the patients experienced major or complete pain relief that lasted upon follow-up ranging from 3 to 11 years. Helliwell also observed patients whereby 44% experienced complete pain relief, and 45% had moderate or substantial pain relief. Friberg found that 157 (of 211) patients with LBP, treated with shoe lifts, were symprom-free after a mean follow-up of 18 months.

leg length discrepancy measurement
Surgical Treatment
Leg shortening is employed when LLD is severe and when a patient has already reached skeletal maturity. The actual surgery is called an osteotomy , which entails the removal of a small section of bone in the tibia (shinbone) and sometimes the fibula as well, resulting in the loss of around an inch in total height. Leg lengthening is a difficult third option that has traditionally had a high complication rate. Recently, results have improved somewhat with the emergence of a technique known as callotasis , in which only the outer portion of the bone (the cortex ) is cut, (i.e. a corticotomy ). This allows the bone to be more easily lengthened by an external fixation device that is attached to either side of the cut bone with pins through the skin. The ?ex-fix,' as it is sometimes called, is gradually adjusted by an orthopaedic surgeon, and healing can occur at the same time that the leg is being distracted , or lengthened over time. Unlike epiphysiodesis, leg lengthening procedures can be performed at almost any skeletal or chronological age.
Mortons Neuroma Causes
Overview
 Morton's neuroma, also called Morton's metatarsalgia, Morton's disease, Morton's neuralgia, Morton metatarsalgia, Morton nerve entrapment, plantar neuroma, or intermetatarsal neuroma is a benign (non-cancerous) growth of nerve tissue (neuroma) that develops in the foot, usually between the third and fourth toes (an intermetatarsal plantar nerve, most commonly of the third and fourth intermetatarsal spaces). It is a common, painful condition.
Morton's neuroma, also called Morton's metatarsalgia, Morton's disease, Morton's neuralgia, Morton metatarsalgia, Morton nerve entrapment, plantar neuroma, or intermetatarsal neuroma is a benign (non-cancerous) growth of nerve tissue (neuroma) that develops in the foot, usually between the third and fourth toes (an intermetatarsal plantar nerve, most commonly of the third and fourth intermetatarsal spaces). It is a common, painful condition.
Causes
It's not always clear what causes Morton's neuroma, but several things seem to aggravate it. These include other foot-related problems and wearing restrictive footwear. It's thought that Morton's neuroma may be caused by the toe bones (metatarsal bones) pressing against the nerve when the gap between the bones is narrow. This causes the nerve and surrounding tissue to thicken.
Symptoms
Morton's neuroma can cause a very painful burning or sharp pain in your foot that feels worse when you walk. It may feel like a small lump inside the ball of your foot. It is usually between the third and fourth toes, but it can also be between other toes.
Diagnosis
If you suspect Morton?s Neuroma, it is essential that you confirm your suspicions by consulting with a podiatric physician. Don?t wait for the symptoms to go away for good (even if they tend to come and go). Also, remember that many conditions have similar symptoms, and only a professional can tell the difference.
Non Surgical Treatment
Rest. Continuing with normal training will increase pain and inflammation and prevent the injury from healing. Wear a metatarsal pad under the forefoot which will raise and spread the bones of the forefoot taking the pressure off the nerve. Wearing metatarsal pads in the shoes under the forefoot spreads the metatarsals creating more space for the nerve. See a sports injury professional who can advise on treatment and rehabilitation. Orthotic inserts may be required to correct any biomechanical dysfunction of the foot.
Surgical Treatment
Surgery is occasionally required when the conservative treatment is not able to relieve your symptoms, particularly if you have had pain for more than 6 months. 80% of patients who require surgery report good results, with 71% of people becoming pain-free.
Prevention
To help reduce your chance of developing Morton's neuroma avoid wearing tight and/or high-heeled shoes. Maintain or achieve ideal body weight. If you play sports, wear roomy, properly fitting athletic footwear.
 Morton's neuroma, also called Morton's metatarsalgia, Morton's disease, Morton's neuralgia, Morton metatarsalgia, Morton nerve entrapment, plantar neuroma, or intermetatarsal neuroma is a benign (non-cancerous) growth of nerve tissue (neuroma) that develops in the foot, usually between the third and fourth toes (an intermetatarsal plantar nerve, most commonly of the third and fourth intermetatarsal spaces). It is a common, painful condition.
Morton's neuroma, also called Morton's metatarsalgia, Morton's disease, Morton's neuralgia, Morton metatarsalgia, Morton nerve entrapment, plantar neuroma, or intermetatarsal neuroma is a benign (non-cancerous) growth of nerve tissue (neuroma) that develops in the foot, usually between the third and fourth toes (an intermetatarsal plantar nerve, most commonly of the third and fourth intermetatarsal spaces). It is a common, painful condition.Causes
It's not always clear what causes Morton's neuroma, but several things seem to aggravate it. These include other foot-related problems and wearing restrictive footwear. It's thought that Morton's neuroma may be caused by the toe bones (metatarsal bones) pressing against the nerve when the gap between the bones is narrow. This causes the nerve and surrounding tissue to thicken.
Symptoms
Morton's neuroma can cause a very painful burning or sharp pain in your foot that feels worse when you walk. It may feel like a small lump inside the ball of your foot. It is usually between the third and fourth toes, but it can also be between other toes.
Diagnosis
If you suspect Morton?s Neuroma, it is essential that you confirm your suspicions by consulting with a podiatric physician. Don?t wait for the symptoms to go away for good (even if they tend to come and go). Also, remember that many conditions have similar symptoms, and only a professional can tell the difference.
Non Surgical Treatment
Rest. Continuing with normal training will increase pain and inflammation and prevent the injury from healing. Wear a metatarsal pad under the forefoot which will raise and spread the bones of the forefoot taking the pressure off the nerve. Wearing metatarsal pads in the shoes under the forefoot spreads the metatarsals creating more space for the nerve. See a sports injury professional who can advise on treatment and rehabilitation. Orthotic inserts may be required to correct any biomechanical dysfunction of the foot.

Surgical Treatment
Surgery is occasionally required when the conservative treatment is not able to relieve your symptoms, particularly if you have had pain for more than 6 months. 80% of patients who require surgery report good results, with 71% of people becoming pain-free.
Prevention
To help reduce your chance of developing Morton's neuroma avoid wearing tight and/or high-heeled shoes. Maintain or achieve ideal body weight. If you play sports, wear roomy, properly fitting athletic footwear.
Shoe Lifts For Leg Length Discrepancy
There are actually not one but two different kinds of leg length discrepancies, congenital and acquired. Congenital means you are born with it. One leg is structurally shorter compared to the other. Through developmental stages of aging, the brain senses the step pattern and recognizes some difference. Our bodies typically adapts by tilting one shoulder to the "short" side. A difference of under a quarter inch is not grossly abnormal, does not need Shoe Lifts to compensate and normally won't have a serious effect over a lifetime.

Leg length inequality goes typically undiagnosed on a daily basis, yet this problem is very easily remedied, and can reduce numerous cases of back ache.
Therapy for leg length inequality commonly involves Shoe Lifts. Many are cost-effective, usually costing below twenty dollars, compared to a custom orthotic of $200 or more. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position.
Lower back pain is easily the most common ailment impacting people today. Over 80 million men and women suffer from back pain at some point in their life. It's a problem that costs businesses millions annually on account of time lost and output. New and improved treatment methods are continually sought after in the hope of minimizing the economic impact this issue causes.

People from all corners of the world experience foot ache due to leg length discrepancy. In most of these cases Shoe Lifts might be of immense help. The lifts are capable of alleviating any pain and discomfort in the feet. Shoe Lifts are recommended by countless expert orthopaedic practitioners".
In order to support the human body in a balanced fashion, feet have a significant task to play. In spite of that, it is sometimes the most neglected region in the human body. Many people have flat-feet meaning there may be unequal force placed on the feet. This causes other parts of the body like knees, ankles and backs to be impacted too. Shoe Lifts guarantee that the right posture and balance are restored.

Leg length inequality goes typically undiagnosed on a daily basis, yet this problem is very easily remedied, and can reduce numerous cases of back ache.
Therapy for leg length inequality commonly involves Shoe Lifts. Many are cost-effective, usually costing below twenty dollars, compared to a custom orthotic of $200 or more. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position.
Lower back pain is easily the most common ailment impacting people today. Over 80 million men and women suffer from back pain at some point in their life. It's a problem that costs businesses millions annually on account of time lost and output. New and improved treatment methods are continually sought after in the hope of minimizing the economic impact this issue causes.

People from all corners of the world experience foot ache due to leg length discrepancy. In most of these cases Shoe Lifts might be of immense help. The lifts are capable of alleviating any pain and discomfort in the feet. Shoe Lifts are recommended by countless expert orthopaedic practitioners".
In order to support the human body in a balanced fashion, feet have a significant task to play. In spite of that, it is sometimes the most neglected region in the human body. Many people have flat-feet meaning there may be unequal force placed on the feet. This causes other parts of the body like knees, ankles and backs to be impacted too. Shoe Lifts guarantee that the right posture and balance are restored.
The Diagnosis Of Inferior Calcaneal Spur
Overview
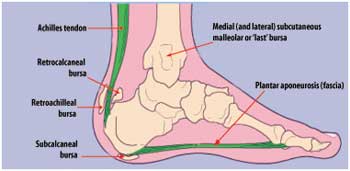
Heel spurs are tiny protruding calcium deposits that can develop near the base of your heel bone. They can be caused by repetitive activities, such as dancing or running, or they can form in association with plantar fasciitis, which is an inflammation of the ligament (plantar fascia) on the bottom of your foot. When the plantar fascia is tight and pulls on your heel bone, the bone releases calcium to try to heal itself. The excess deposits of calcium can sometimes form heel spurs.
Causes
The calcaneal spur is seen most often in persons over the age of 40. The condition can also be associated with osteoarthritis, rheumatoid arthritis, poor circulation of the blood and other degenerative diseases. Men and women are equally likely to have them.

Symptoms
With heel spurs, people often talk about a dull ache which is felt most of the time with episodes of a sharp pain in the center of the heel or on the inside margin of the heel. Often the pain is worse on first rising in the morning and after rest and is aggravated by prolonged weight bearing and thin-soled shoes.
Diagnosis
A heel spur is often seen on X-ray as a bony protrusion, which can vary in size. However, because a Heel Spur only indicates increased load on the plantar fascia, and not pain, an ultra sound may be required to assess other actual cause of the heel pain such and may include checking to see if the plantar fascia is inflamed or degenerated.
Non Surgical Treatment
If pain and other symptoms of inflammation-redness, swelling, heat-persist, you should limit normal daily activities and contact a doctor of podiatric medicine. The podiatric physician will examine the area and may perform diagnostic X-rays to rule out problems of the bone. Early treatment might involve oral or injectable anti-inflammatory medication, exercise and shoe recommendations, taping or strapping, or use of shoe inserts or orthotic devices. Taping or strapping supports the foot, placing stressed muscles and tendons in a physiologically restful state. Physical therapy may be used in conjunction with such treatments. A functional orthotic device may be prescribed for correcting biomechanical imbalance, controlling excessive pronation, and supporting of the ligaments and tendons attaching to the heel bone. It will effectively treat the majority of heel and arch pain without the need for surgery. Only a relatively few cases of heel pain require more advanced treatments or surgery. If surgery is necessary, it may involve the release of the plantar fascia, removal of a spur, removal of a bursa, or removal of a neuroma or other soft-tissue growth.
Surgical Treatment
In some cases, heel spurs are removed by surgery after an X-ray. While the surgery is typically effective, it?s a timely and expensive procedure. Even after surgery, heel spurs can re-form if the patient continues the lifestyle that led to the problem. These reasons are why most people who develop painful heel spurs begin looking for natural remedies for joint and bone pain. Surgery isn?t required to cure a heel spur. In fact, more than 90 percent of people get better with nonsurgical treatments. If nonsurgical methods fail to treat symptoms of heel spurs after 12 months, surgery may be necessary to alleviate pain and restore mobility.
Prevention
A variety of steps can be taken to avoid heel pain and accompanying afflictions. Wear shoes that fit well-front, back, and sides-and have shock-absorbent soles, rigid shanks, and supportive heel counters. Wear the proper shoes for each activity. Do not wear shoes with excessive wear on heels or soles. Prepare properly before exercising. Warm up and do stretching exercises before and after running. Pace yourself when you participate in athletic activities. Don't underestimate your body's need for rest and good nutrition. If obese, lose weight.
What Is A Heel Spur

Overview
A heel spur is a hooked bony growth protruding from the calcaneus or heel bone. It often occurs alongside plantar fasciitis, and as such the two conditions are often confused, however they are not the same.
Causes
A strong band of sinew (plantar fascia) stretches across the sole of the foot below the surface of the skin and is attached to a point in the middle of the under surface of the heel bone. With repeated activity on our feet, the plantar fascia can become tight and cause persistent traction (tugging) on its attachment point into the heel bone, and inflammation and pain may develop at this site. This painful condition is known as plantar fasciitis. Sometimes a ?spur? develops at the site of this traction on the bone and protrudes into the surrounding tissue. This is a heel spur.
.gif)
Symptoms
Heel spurs are most noticeable in the morning when stepping out of bed. It can be described as sharp isolated pain directly below the heel. If left untreated heel spurs can grow and become problematic long-term.
Diagnosis
Your doctor, when diagnosing and treating this condition will need an x-ray and sometimes a gait analysis to ascertain the exact cause of this condition. If you have pain in the bottom of your foot and you do not have diabetes or a vascular problem, some of the over-the-counter anti-inflammatory products such as Advil or Ibuprofin are helpful in eradicating the pain. Pain creams, such as Neuro-eze, BioFreeze & Boswella Cream can help to relieve pain and help increase circulation.
Non Surgical Treatment
Some heel spurs do require surgery, however surgery is a last resort. In most cases the patients underlying foot problem needs to be addressed, such as Over Pronation and Over Supination and Heel Pain Treatment Options need to be implemented if Plantar Fasciitis and Achilles Tendonitis are still an ongoing concern. Your best treatment is always prevention.
Surgical Treatment
Surgery, which is a more radical treatment, can be a permanent correction to remove the spur itself. If your doctor believes that surgery is indicated, he will recommend an operation - but only after establishing that less drastic methods of treatment are not successful.